Thinking about trying one of the new weight-loss drugs? You’re not alone — these medications have turned into the latest toolbox in the battle against extra pounds. But before you sign up for the shot (or the future pill), here’s a friendly, slightly cheeky guide to what to expect, how they work, and why they’re not a magical erase-button.
What these drugs actually do
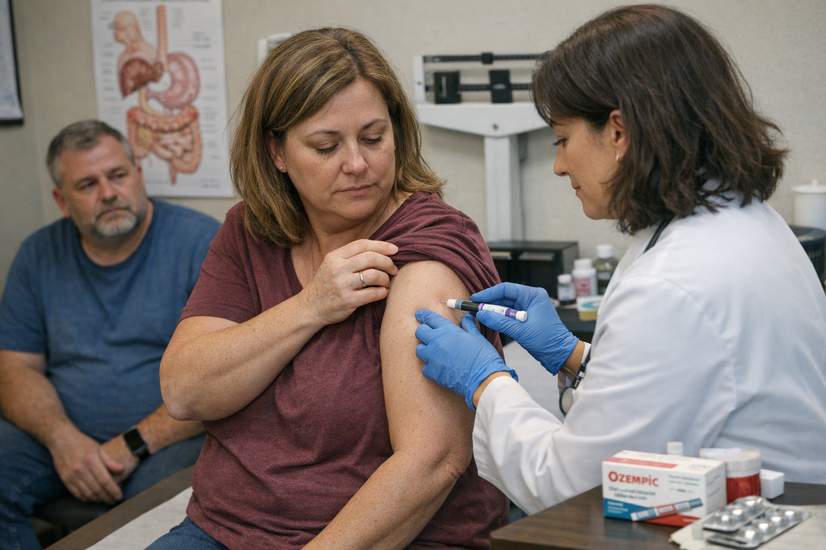
Drugs like semaglutide and tirzepatide (you may know them by brand names such as Ozempic and Mounjaro) mainly shut down your appetite by copying hormones that tell the brain you’re full. They latch onto GLP‑1 and GIP receptors and make food feel less tempting — which, yes, can make eating less of a drama.
Results can be impressive: many people lose double-digit percentages of body weight over months. But not everyone responds the same way — roughly one in ten to one in seven people see very little change.
Don’t expect a forever fix if you stop
One of the biggest surprises for people is how fast weight can come back once the medication stops. Studies show weight tends to rebound much more quickly after stopping these drugs than after stopping a behaviour-based weight-loss program. In some research, people regained substantial portions of their lost weight within months after quitting.
Why? Biology is a drama queen. Your body ramps up hunger hormones and slows your metabolism to try to bring weight back, while constant food cues in modern life (ads, food delivery, snack aisles) keep whispering temptations in your ear. That’s why many people end up needing long-term treatment or ongoing support.
It’s not just the drug — lifestyle still matters
A fair number of people do make meaningful lifestyle changes while on medication and can reduce their dose or take breaks. But the majority will likely still need some level of pharmacological help, simply because the world doesn’t stop offering ultra-tempting, high-calorie foods.
Experts warn that relying solely on medication without dietary and behavioural support can cause problems: rapid appetite reduction may mean people eat less but not necessarily better, which raises the risk of poor nutrient intake, muscle loss, or other unintended outcomes. So if you use these drugs, aim to pair them with guidance on food quality, protein intake, and activity.
Small nudges add up
Researchers have experimented with tiny, doable habit changes — think swapping a sugary drink for water, stepping outside for five minutes, or breathing through stress — and found these “microsteps” help people build confidence and momentum. They’re low-effort, low-risk moves that stack up into real wins over time, especially when you’re also benefiting from appetite suppression.
Side effects and unknowns
Common side effects are usually digestive — nausea, stomach discomfort, that sort of thing. There are also signals linking these drugs to pancreatitis, gallstones, muscle loss if people aren’t active enough, and possible effects on bones and joints. We also don’t have a full picture of very long-term effects or impacts on pregnancy and future children, so people who are pregnant (or trying to be) need to be cautious.
That said, for many people with weight-related health problems, the benefits (improvements in blood pressure, sleep apnea, and other conditions) can outweigh the risks — but that trade-off is personal and should be discussed with a clinician.
The bigger picture: drugs are a tool, not a total solution
These medications are a major development and can be life-changing for some. But public-health experts remind us that medication alone won’t solve the obesity problem. Better food environments, earlier intervention, and broader support systems are still essential if we want long-term change on a population level.
Think of the drugs as a powerful assist: they make it easier to eat less and think about health, but the best outcomes come when pharmacology teams up with good food, movement, and sustainable habits.
Bottom line
If you’re considering weight-loss medication: do your homework, talk to a clinician about risks and realistic expectations, plan for lifestyle support, and be prepared for the possibility that stopping the drug could bring back weight. They’re exciting tools, but not magic; a sensible plan and ongoing support will get you much farther than relying on the shot alone.