Quick elevator pitch
Ibogaine is a powerful psychedelic derived from an African shrub that’s mostly illegal in many countries. Lately it’s been getting attention because some veterans and people with addictions say a single supervised session felt like a reset — easing PTSD symptoms, cutting cravings and, in a few cases, changing lives. Scientists are intrigued but confused: is it the brain chemistry or the psychedelic trip (or both) doing the healing?
A veteran takes a gamble
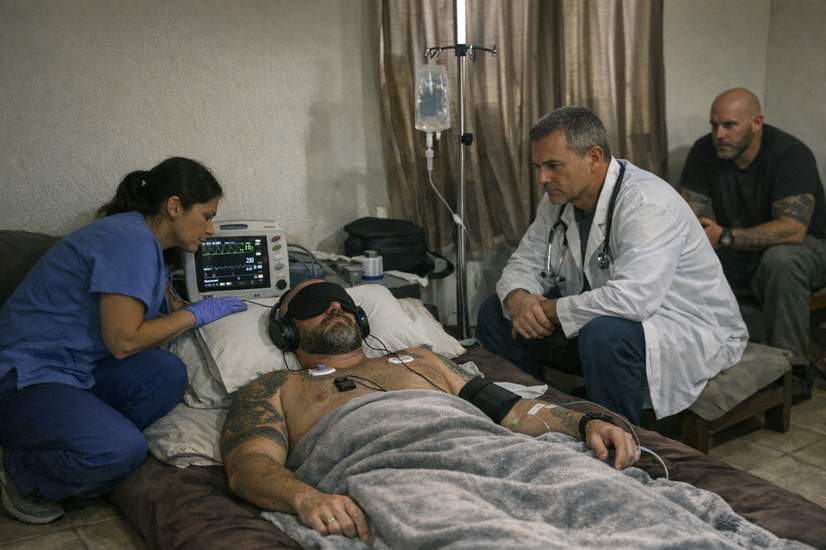
One former US special-operations medic reached a point where traditional treatments and dozens of surgeries didn’t bring relief. Desperate for a different option, he travelled to a clinic where ibogaine is legal and signed up for a monitored session. Lying on a mat with eyeshades on, he spent many hours inside intense memory-like experiences that felt startlingly real — revisiting people and scenes from his past and confronting old pain.
How the Mexico sessions were run
In the trial, small groups of veterans were given measured doses over a few hours and watched by medical staff. Participants were prepped for long, dreamlike journeys and kept under supervision through the acute effects. After a single experience, many reported fewer PTSD symptoms and improvements in mood and anxiety on follow-up questionnaires.
Ibogaine’s stranger origin story
Interest in ibogaine isn’t new. Informal reports decades ago suggested it could blunt drug withdrawal, sparking research into addiction and mood effects. Over the years, small studies and clinic reports have repeatedly hinted that it can interrupt cravings and create powerful psychological shifts for some people.
How might it work? The messy science
Ibogaine isn’t a run-of-the-mill psychedelic. It interacts with several brain systems and produces a metabolite called noribogaine that seems to affect serotonin and other circuits. Some evidence points to effects on receptors linked to myelin repair and to increases in growth factors that help brain cells rewire — a process that could mend damage from addiction or trauma.
Trip, chemistry, or both?
Researchers are split. A few labs created versions of the compound that don’t induce hallucinations but still produced benefit in animal tests, suggesting chemistry alone might matter. Other teams argue the vivid, often cathartic visionary experience — the replaying of memories, the emotional processing — is central, because intensity of the trip has correlated with better outcomes in some studies. The honest answer right now is: probably some of each.
Brain waves, dreams, and rewiring
Measurements of brain activity from treated veterans show changes that resemble deeper emotional processing — decreased activity in certain brain rhythms linked to PTSD, and signals consistent with more flexible thinking. People often describe the experience like watching a movie of their life from a new angle, which can let them reinterpret old patterns and create healthier responses.
Not a magic bullet
Ibogaine isn’t universally effective. Some patients report no benefit or even worsened outcomes, and the treatment can be dangerous — there are documented cardiac risks and a handful of fatalities linked to unsupervised use. Clinics that run these programs typically screen heavily, provide continuous medical monitoring, and sometimes use protective measures like magnesium infusions to reduce heart risks.
Practical problems: cost, legality and follow-up
Because ibogaine is illegal in many places, most data comes from a few clinics abroad and from small studies, making it hard to draw firm conclusions. Treatment is expensive, medically intensive and often paired with other psychedelics or therapies, which complicates understanding which element is doing the work. Larger, well-controlled trials and better safety tracking are needed before it could become mainstream.
Who seems to benefit?
Some veterans and people struggling with addiction say the change feels dramatic — reduced pain, calmer minds, fewer cravings — but they also emphasise that the drug is only part of the story. Sustainable improvement usually involves follow-up: therapy, journaling, meditation and ongoing effort to apply whatever insights the experience revealed.
Where things are headed
Research interest and funding for psychedelic science have been growing, and ibogaine is part of that wave. Scientists are racing to pin down mechanisms, improve safety, and test non-hallucinogenic analogues. Until then, the picture is hopeful but incomplete: a fascinating compound with rare promise, real risks, and a ton of unanswered questions.